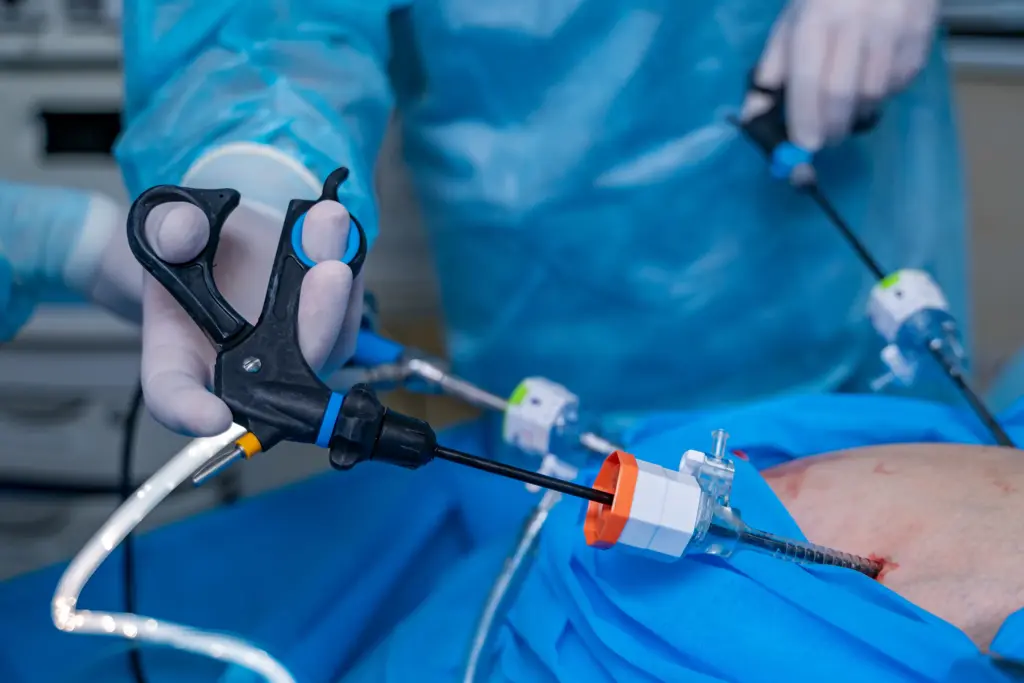
Laparoscopic surgery: Laparoscopy uses a camera and slim instruments through tiny skin cuts (“ports”), typically under general anaesthesia. For most patients, it means less pain, smaller scars, faster recovery, but good outcomes still depend on preparation, realistic expectations, and disciplined aftercare.
Before surgery: smart preparation (7–14 days out)
Tests & fitness. You’ll usually have blood work, ECG/chest X-ray as needed, and anaesthesia review. Tell your team about sleep apnoea (bring your CPAP), prior reactions to anaesthesia, and any bleeding tendency.
Also Read | Our Expert Article: Dr Ronak Malani on Colon Cancer’s Red Flags
Medicines to review (only change with your doctor’s advice):
- Blood thinners/antiplatelets: may need pausing or bridging.
- Diabetes meds: insulin/tablets are adjusted the night before and morning of surgery.
- Herbals/supplements: stop those that increase bleeding (e.g., ginseng, gingko).
- Painkillers: Avoid NSAIDs if your surgeon advises.
Smoking: Stop smoking & vaping/nicotine, even 2–4 weeks off lowers lung and wound risks. Prioritise sleep, hydration, and protein-rich meals (dal, eggs, paneer, fish) to aid healing.
Fasting (as per anaesthesia): no solid food for 6–8 h; clear liquids allowed up to 2 h before, unless instructed otherwise.
Logistics: Arrange an adult escort home, 48–72 h of home help, and sick-leave approval. For women of childbearing age, a pregnancy test is standard on the day.
On the day: what actually happens
You’ll sign consent (including the small chance of conversion to open surgery for safety). In theatre, we inflate the abdomen with CO2 to create working space; this explains the common shoulder-tip pain afterwards (phrenic nerve irritation). Many laparoscopic procedures are performed on an outpatient basis or require an overnight stay.
Expect a sore throat from the breathing tube, mild bloating, and drowsiness. We start oral fluids early and encourage first steps within hours.
Scars & cosmetic results: what to expect (and how to help them heal)
Incisions & placement:
- One umbilical port (10–12 mm) for the camera.
- Two to three working ports (5–8 mm) on the abdomen’s sides or lower belly.
- Some operations use a single hidden umbilical incision; robotic surgery uses similar sizes but may add one extra port.
- Closure. Deeper layers are stitched; skin is closed with absorbable sutures, skin glue or Steri-Strips.
Appearance over time:
- Week 1–2: pink lines with mild bruise/itch.
- Week 3–8: colour can darken in Indian skin; firmness is normal.
- Months 3–12: scars flatten and fade. If you have a history of hypertrophic/keloid scars, tell your surgeon; silicone gel/sheets for 8–12 weeks, gentle scar massage (after wounds are sealed), and daily sunscreen on exposed areas improve outcomes.
- Port-site hernia risk is low but higher at =10–12 mm sites. Avoid heavy lifts until cleared.
Recovery: realistic timelines (guide, not a rulebook)
Shared early tips (first 3–5 days)
- Walking every few hours reduces gas pain and DVT risk.
- Use prescribed pain control (usually paracetamol + anti-spasmodic; short opioids only if needed).
- Micronutrition: 60–80 g/day of protein if possible; hydrate well.
- Bowel care: stool softener to prevent straining.
- Showers: usually allowed after 24–48 h; pat incisions dry; no tub/soak till cleared.
- Driving: only when you can emergency-brake comfortably and are off opioids (often 48–72 h for minor procedures).
Procedure-specific ranges (typical, uncomplicated cases):
- Diagnostic laparoscopy / ovarian cystectomy/endometriosis ablation: Desk work 3–5 days; gym/weights 3–4 weeks.
- Laparoscopic cholecystectomy (gallbladder): Light routine 3–5 days; desk 5–7 days; heavy labour 4 weeks.
- Laparoscopic appendectomy (simple): Desk 3–5 days; heavy work 3–4 weeks.
- Laparoscopic inguinal/ventral hernia repair: Desk 3–7 days; no lifting >5–7 kg for 4–6 weeks; core training re-starts gradually after clearance.
- Laparoscopic hysterectomy / major colorectal resections: Desk 2–3 weeks (hysterectomy) / 2–4 weeks (colorectal); strenuous work 6–8 weeks.
- Sex & intimacy: when comfortable if no vaginal surgery; after hysterectomy or pelvic repairs, your gynae team will usually advise 4–6 weeks.
- Flights: short haul after 1 week if uncomplicated; long haul 2–3 weeks with in-flight walking and compression stockings (confirm with your surgeon).
Diet after laparoscopy (practical)
Start with clear liquids and a soft diet. After gallbladder surgery, keep meals small and low-fat for 1–2 weeks while bile flow adapts. Gas-forming foods (carbonated drinks, very spicy/fried meals) can worsen bloating early on.
Wound care & warning signs
Call your team urgently for:
- Keep dressings as advised; change only if wet/soiled.
- Fever =38 °C, worsening abdominal pain or swelling
- Red, hot, pus-like discharge from any port
- Persistent vomiting, inability to pass urine or stools
- Jaundice (after gallbladder/bile duct work)
- Calf pain/swelling, sudden breathlessness (possible clot)
- New bulge at a port site with pain (possible port-site hernia)
- Observe edges: they should be closed, not gaping.
Also Read | Our Expert Article: Dr Nilay Desai on Can You Outrun Family Diabetics
FAQs I answer every week
- “Why does my shoulder hurt?”
CO2 irritates the diaphragm; walking, heating pad, anti-spasmodics, and time help (24–72 h). - “My belly feels bloated.”
Common for 3–7 days; keep moving, sip fluids, avoid fizzy drinks, use stool softeners. - “When can I remove Steri-Strips?”
Usually, day 7–10 or when they loosen on their own, unless your surgeon says otherwise. - “Can laparoscopy leave no scar at all?”
Scars are permanent but can be discreet; silicone therapy and sun protection optimise fading. Some skin types (including darker tones) are more prone to hyperpigmentation or hypertrophy—plan preventive care early.
Your one-page checklist
- Tests done; anaesthesia review completed
- Medicines reviewed (blood thinners/diabetes/herbals)
- Fasting & arrival time confirmed
- Protein-first meals this week; stopped smoking
- Escort and 72-hour home help arranged
- Pain, stool softener, and dressing supplies at home
- Follow-up appointment on calendar (usually 7–14 days)
Laparoscopy is designed for quicker, cleaner recovery, but it still demands good prep, early movement, disciplined wound care, and respect for lifting limits. If you follow the plan and report red flags early, most patients return to normal life within days to a few weeks, with small, well-healed scars to show for it.
Medical disclaimer: This article is for general education and does not replace a personalised consultation. Timelines vary by procedure, findings, and your health status. Always follow your own surgeon and anaesthesia team’s instructions.